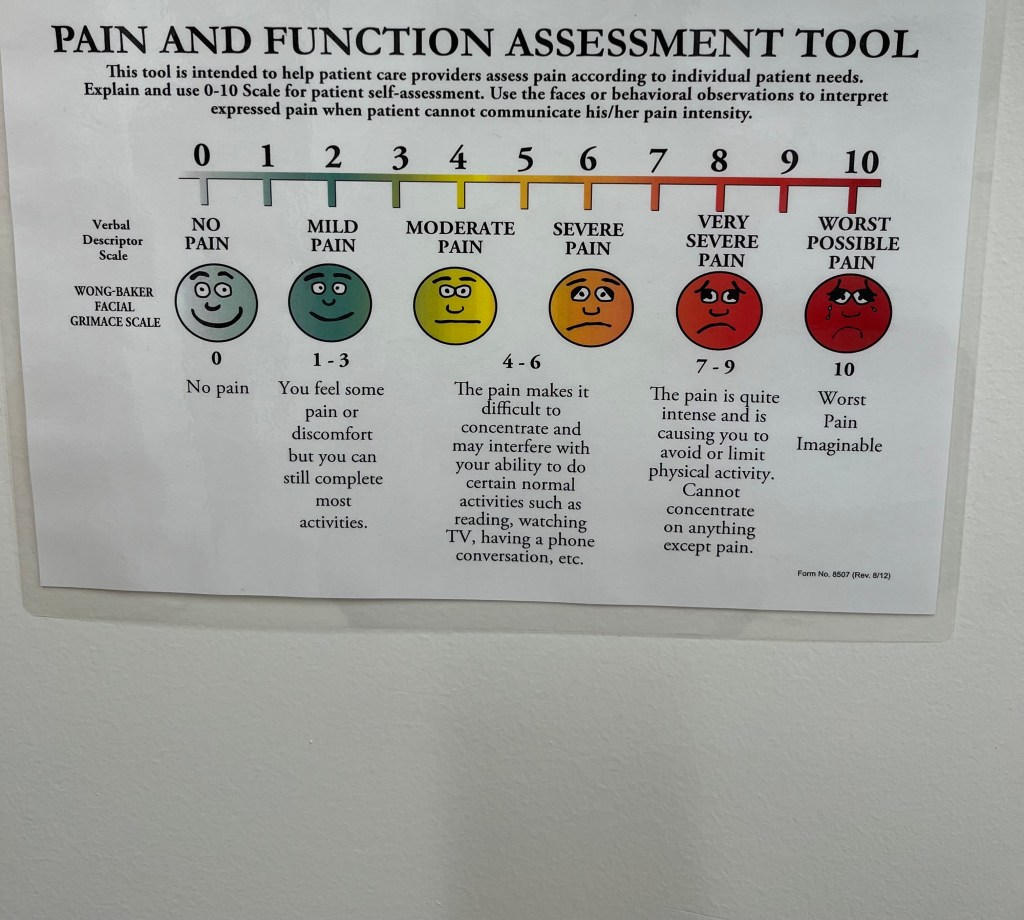
The nurse called my name and walked with me from the waiting room to the exam room. In the exam room, she had me step on the scale, and she checked my temperature and blood pressure. And while she stood at the computer, inputing the numbers, she asked me what my pain was like today.
This was about 9:30 am Tuesday morning. My pain was bad. But, the day before had been worse. After waking up to my 6:00 am alarm, I had made the bed, brushed my teeth and washed my face, gotten dressed, and come downstairs. Moving around I felt stiff. Standing up brushing my teeth, I put my weight on my right leg and foot. My left side felt weak, like it might give out. I knew it would be hard to walk down the flight of stairs to our living room and kitchen. I hadn’t expected to be crying before I reached the final step.
Tuesday morning, appointment morning, there were no tears. Grimaces. Limps. Slow, laborious movements. But no tears. So technically I guess the pain was better, but it was still friggin awful.
“It’s a hard question to answer when you live with chronic pain,” I told her.
She didn’t look up.
I tried waiting her out.
She wanted a number. I finally told her 7.
Was it a 7? I don’t know. I know my left leg felt pressure, as if something heavy was placed on my lap. My left calf felt tight, like it was stuck in almost-muscle cramp. I know getting in and out of my car wasn’t all quick, graceful moments but more like slow, intentional movements.
When I met with the doctor, we reviewed all my medication, pain-related and otherwise. He told me the goal is to get me functional, so I don’t let the pain stop me from doing things in my life.
Um, hello?
What?
“To get me functional?”
“So pain doesn’t stop me?” Most people who know me know that isn’t the case.
Perhaps my favorite question was, “when did the pain start?”
I told him the truth. “2010.”
And, as if all that wasn’t bad enough, the doctor asked me his own pain-rating question. Except he didn’t want to know my current pain. Instead he asked, “What would you say was the average for the pain you experienced last week?”
A whole week? I have no idea, and that’s what I told him. My pain fluctuates. Pain can start off feeling incredibly intense and gradually ease up as the day goes on. And the flip side of that is also true — pain can be moderate and then, while doing one of my physical therapy exercises at home for example, something gets triggered and I need an ice pack on my knee, and I’m feeling much worse than I was.
Most frustrating was that my appointment was with a pain management group. These are healthcare providers who work with patients who live with chronic pain. And they should know that if you suffer from chronic pain, you’re looking at that pain scale very differently than someone who is dealing with acute pain.
Acute pain is temporary. It’s pain that is caused by the result of something specific — an accident or injury of some kind, like falling down or getting hurt while playing a sport. But the key word is temporary. Acute pain won’t last. It will impact your daily life, but not forever.
Chronic pain, however, is long-lasting and difficult to treat. What works for one person might not work for another. And what worked for me three years ago may not work for me now.
The doctor told me that no pain medication is going to make the pain go away completely. But the goal is for the pain medication to make a significant difference in my life so that my pain doesn’t stop me from doing what I want and/or need to do.
“We don’t want your pain to stop you from being functional,” the doctor said.
I looked at the doctor in dismay. Shock. Disgust. Impatience. Probably a combination of all of those.
I told him what I have told other doctors — I think when you live with pain for a long time, you get good at pushing through. You have to learn to live with the pain, alongside the pain, if you’re planning on living your life as fully as you can.
The truth is no one can really know what my pain feels like. We each experience pain in our own way. However, I am convinced that those of us living with chronic pain, exercise a specific set of muscles. My pain level 6 would be someone else’s level 9.
Those of us living with chronic pain have more than enough to deal with. I think we deserve a great deal of respect for all we do, including going in to see a doctor. That by itself is a big deal.
And if I could ask healthcare providers for one change:
Please oh please, stop making patients use an emoji-like pain scale to describe our pain.